주메뉴
- About IBS 연구원소개
-
Research Centers
연구단소개
- Research Outcomes
- Mathematics
- Physics
- Center for Underground Physics
- Center for Theoretical Physics of the Universe (Particle Theory and Cosmology Group)
- Center for Theoretical Physics of the Universe (Cosmology, Gravity and Astroparticle Physics Group)
- Dark Matter Axion Group
- Center for Artificial Low Dimensional Electronic Systems
- Center for Quantum Nanoscience
- Center for Exotic Nuclear Studies
- Center for Van der Waals Quantum Solids
- Center for Relativistic Laser Science
- Center for Trapped Ion Quantum Science
- Chemistry
- Life Sciences
- Center for Memory and Glioscience (Cognitive Glioscience Group)
- Center for Memory and Glioscience (Learning and Memory Group)
- Center for Synaptic Brain Dysfunctions
- Center for RNA Research
- Center for Genomic Integrity
- Center for Vascular Research
- Center for Genome Engineering
- Center for Microbiome–Body–Brain Physiology
- Earth Science
- Interdisciplinary
- Center for Neuroscience Imaging Research (Neuro Technology Group)
- Center for Neuroscience Imaging Research (Cognitive and Computational Neuroscience Group)
- Center for Algorithmic and Robotized Synthesis
- Center for Nanomedicine
- Center for Biomolecular and Cellular Structure
- Center for 2D Quantum Heterostructures
- Institutes
- Korea Virus Research Institute
- News Center 뉴스 센터
- Career 인재초빙
- Living in Korea IBS School-UST
- IBS School 윤리경영


주메뉴
- About IBS
-
Research Centers
- Research Outcomes
- Mathematics
- Physics
- Center for Underground Physics
- Center for Theoretical Physics of the Universe (Particle Theory and Cosmology Group)
- Center for Theoretical Physics of the Universe (Cosmology, Gravity and Astroparticle Physics Group)
- Dark Matter Axion Group
- Center for Artificial Low Dimensional Electronic Systems
- Center for Quantum Nanoscience
- Center for Exotic Nuclear Studies
- Center for Van der Waals Quantum Solids
- Center for Relativistic Laser Science
- Center for Trapped Ion Quantum Science
- Chemistry
- Life Sciences
- Center for Memory and Glioscience (Cognitive Glioscience Group)
- Center for Memory and Glioscience (Learning and Memory Group)
- Center for Synaptic Brain Dysfunctions
- Center for RNA Research
- Center for Genomic Integrity
- Center for Vascular Research
- Center for Genome Engineering
- Center for Microbiome–Body–Brain Physiology
- Earth Science
- Interdisciplinary
- Center for Neuroscience Imaging Research (Neuro Technology Group)
- Center for Neuroscience Imaging Research (Cognitive and Computational Neuroscience Group)
- Center for Algorithmic and Robotized Synthesis
- Center for Nanomedicine
- Center for Biomolecular and Cellular Structure
- Center for 2D Quantum Heterostructures
- Institutes
- Korea Virus Research Institute
- News Center
- Career
- Living in Korea
- IBS School
News Center
New Experimental Drug May Restore Movement After Stroke- Blocking collagen production after stroke prevents neuronal cell death, full recovery observed in paralyzed monkeys - Every stroke begins with a sudden interruption of blood flow in the brain. But what happens afterward—why neurons continue to lose function and die over the following days—has remained one of the most important unanswered questions in neuroscience. A research team led by Director C. Justin LEE at the Center for Memory and Glioscience within the Institute for Basic Science (IBS), in collaboration with Professor RYU Seungjun of Eulji University, has now uncovered a previously unknown mechanism that drives this delayed brain damage. Their findings show that stroke is not only caused by the initial loss of blood flow, but also by a chain reaction within the brain that unfolds over time. In the brain, neurons rely on astrocytes—star-shaped support cells that help maintain the chemical environment and protect neural circuits. After a stroke, astrocytes rapidly respond to injury by forming a structure known as the glial barrier, which has long been thought to protect surrounding tissue. However, the new study shows that this response can take a harmful turn. The researchers found that immediately after a stroke, levels of hydrogen peroxide (H₂O₂), a reactive oxygen molecule, rise sharply in the affected region. This surge triggers astrocytes to undergo a metabolic shift and begin producing large amounts of type I collagen, a structural protein rarely found in the healthy brain. As collagen accumulates, it becomes incorporated into the glial barrier, creating a dense environment that actively promotes neuronal death rather than preventing it. To confirm that collagen plays a direct role in this process, the team first blocked its production by silencing a key gene in astrocytes. When collagen synthesis was suppressed, neuronal death was significantly reduced, demonstrating that this pathway is not merely associated with damage but is a major driver of it. Further experiments showed that collagen can act as a signaling molecule, activating receptors on neurons and triggering a slow degenerative process that unfolds over several days. Co-corresponding author Dr. LEE Boyoung stated, “We elucidated, at the molecular and cellular levels, the mechanism by which reactive oxygen species induce collagen synthesis in astrocytes. This finding provides a crucial clue for understanding the diverse causes of neuronal death and may serve as a foundation for developing treatments not only for stroke, but also for neurodegenerative diseases such as dementia and Parkinson’s disease.” The researchers then asked whether this damaging cascade could be stopped at an earlier stage. Instead of targeting collagen directly, they tested a newly developed drug called KDS12025, which reduces hydrogen peroxide levels and prevents the entire process from being triggered. In mouse models of stroke, the treatment reduced collagen accumulation, prevented the formation of the glial barrier, preserved neuronal function, and restored motor performance. Most strikingly, the drug remained effective even when administered up to two days after stroke onset. This finding is particularly significant because current stroke treatments are typically limited to a narrow “golden time” window of only a few hours. Extending this window from hours to days suggests that brain damage previously thought to be irreversible may still be preventable. To examine whether these effects could translate to more human-like systems, the team applied the same approach to a stroke model in monkeys. Untreated animals were unable to grasp food due to paralysis, while monkeys treated with KDS12025 regained motor function and successfully grasped food in all 10 out of 10 attempts during behavioral testing. The treated animals also showed reduced brain damage and improved overall neurological function. Co-corresponding author Professor RYU Seungjun added, “We propose hydrogen peroxide and collagen as novel therapeutic targets for stroke. By demonstrating efficacy in a non-human primate model rather than only in cells or small animals, we anticipate a substantial reduction in the time required for clinical translation and new hope for patients.” These findings suggest that stroke is not simply a one-time event, but a progressive biological process driven by interactions between different cell types in the brain. By identifying hydrogen peroxide–induced collagen production in astrocytes as a key step in this process, the study provides a new framework for understanding how brain damage develops—and how it might be stopped. Beyond stroke, the mechanism uncovered in this work may also have broader implications for neurological disorders involving oxidative stress and tissue remodeling, including neurodegenerative diseases. The results point toward a new therapeutic strategy: intervening not only at the moment of stroke, but during the critical period afterward when brain cells are still at risk but potentially recoverable. Corresponding author Director C. Justin LEE (IBS) remarked, “By establishing a ‘one-stop research system’ that integrates the entire process—from basic research to drug development and preclinical validation—we have succeeded not only in identifying the root cause of stroke but also in presenting a concrete therapeutic strategy. We will continue to pursue basic science research that directly benefits humanity and society, as exemplified by KDS12025.” The study was published in Cell Metabolism on April 27. 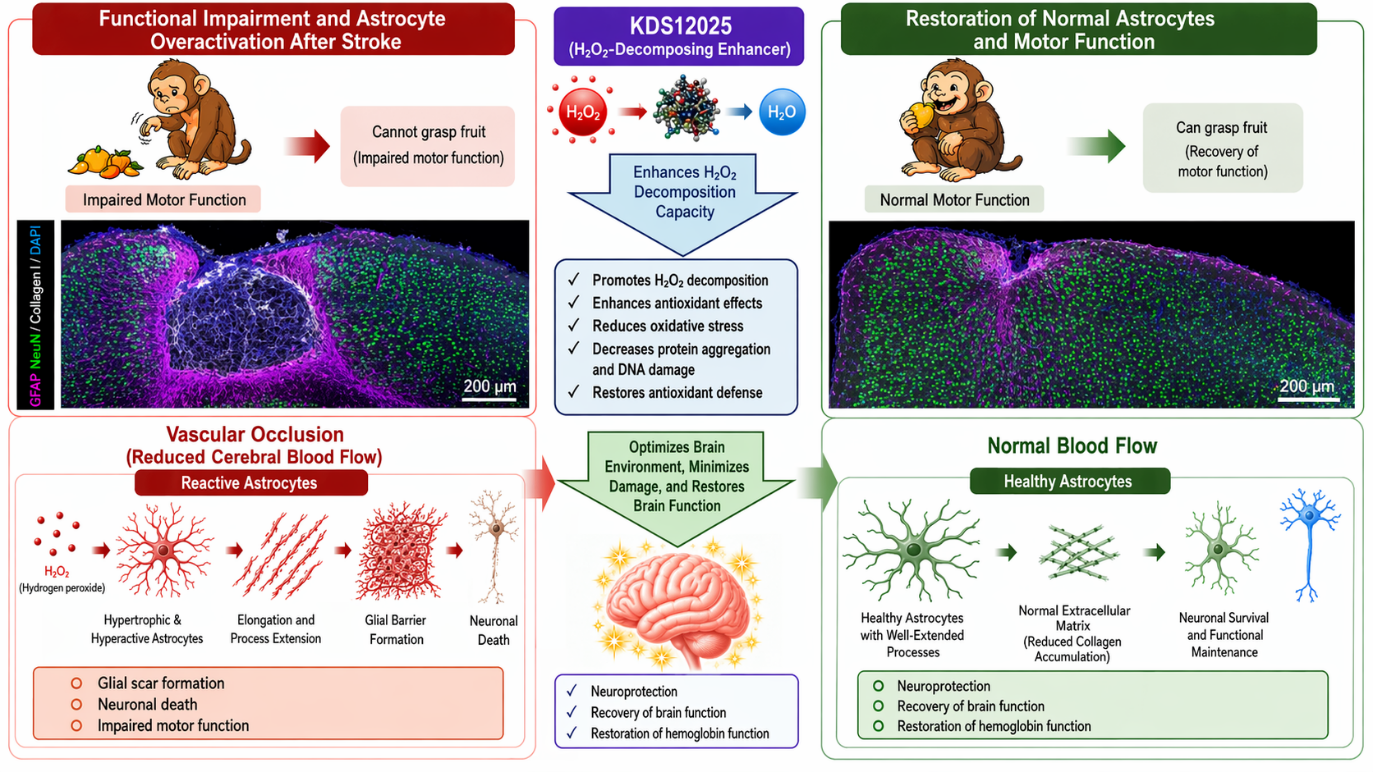 Figure 1. Schematic illustration of astrocyte-derived Type I collagen production and neuronal cell death in ischemic stroke Following ischemic injury, excessive hydrogen peroxide (H₂O₂) is generated, leading to astrocyte activation. Activated astrocytes produce collagen proteins, which contribute to the formation of a glial barrier and induce neuronal cell death. Importantly, inhibition of collagen production or early elimination of excessive hydrogen peroxide prevents the progression of neuronal damage and restores motor function, as demonstrated in non-human primate models. 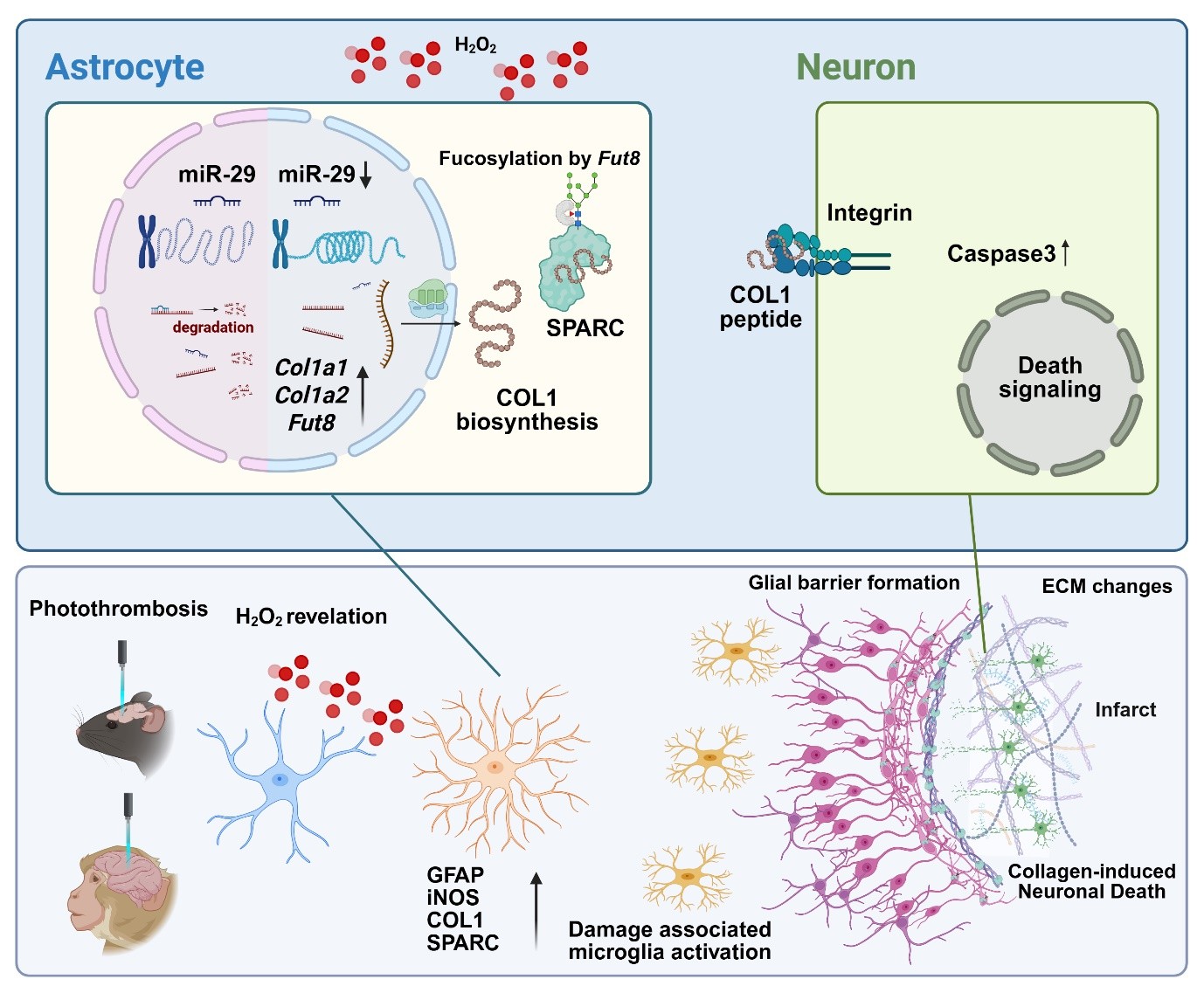 Figure 2. Schematic illustration of astrocyte-derived Type I collagen production and neuronal cell death in ischemic stroke In an ischemic stroke model, excessive hydrogen peroxide (H₂O₂) generated at the early stage activates astrocytes, leading to the production of Type I collagen through gene expression within the cells. The collagen is subsequently secreted into the extracellular space, where it activates microglia, promotes glial barrier formation, and induces neuronal cell death by binding to integrin receptors on neurons. Importantly, suppression of Type I collagen production using viral approaches or early elimination of excessive hydrogen peroxide can prevent the progression of stroke pathology. Notes for editors
- References
- Media Contact
- About the Institute for Basic Science (IBS) |
| before |
|---|
- Content Manager
- Public Relations Team : Suh, William Insang 042-878-8137
- Last Update 2023-11-28 14:20











